If someone is asked to describe their health, they’ll usually say that they’re diabetic. Most people don’t mention whether they have type one or two diabetes. Both conditions cause the body to struggle with glucose storage and usage.
Glucose is used by the body to create energy, and diabetics have an impaired ability to collect the free glucose in the bloodstream, starving the body’s cells of needed energy. The two main types of diabetes have many similarities, but they are different diseases.
Let’s differentiate between them.
Diabetes Type Two (T2D)
T2D is the most common, affecting 90 to 95% of Americans with diabetes. It occurs most often in mature individuals over the age of 45, but teenagers, young adults, and children are being affected, too.
Diabetes type two is when your body can still produce insulin, but the insulin produced is much less useful. You actually become resistant to this hormone that the body needs to regulate your blood glucose levels.
Risk Factors
- Ethnicity plays a huge role in the risk of developing T2D. According to Harvard Medical School, Asian Americans, African Americans, Native Americans, and Hispanics are more likely to develop T2D.
- Genetics is another risk factor. Inheriting certain genes makes you three times more likely to develop diabetes. The main culprit is lipids inside the pancreatic B cell membranes, which cause blockage of the process of storing and converting glucose to energy.
- Obesity is another risk factor for anyone with a body mass index (BMI) of 25 or higher.
- Smoking increases your risk of developing T2D by 30 to 40%.
- A lack of exercise and an unhealthy diet also increases your risk.
- Environmental factors certainly contribute risk.
- T2D might even be the consequence of having too little vitamin D.
- And finally, age certainly plays a big role.
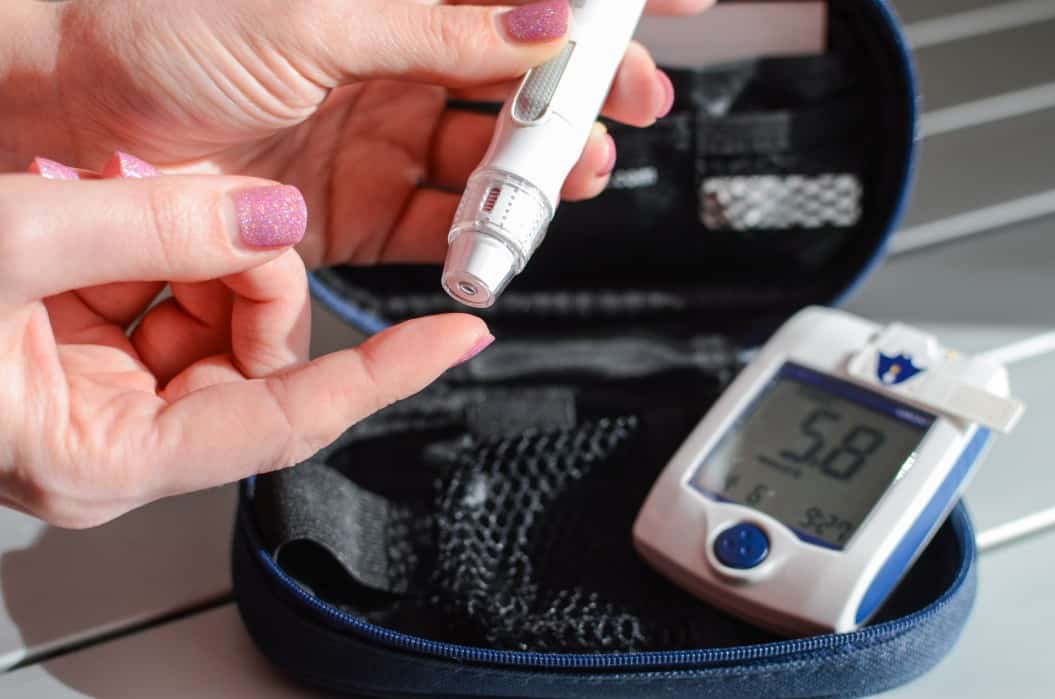
Type One Diabetes (T1D)
T1D only affects around five percent of Americans, and it shares many similarities with T2D, but it develops differently. T1D is an autoimmune disorder, meaning that the immune system attacks and destroys the pancreatic beta cells that produce insulin.
It’s unknown why the immune system attacks the pancreatic cells, but during the process, the pancreas stops making insulin, and supplemental insulin is needed from that time on. Symptoms of T1D appear much faster and are much more profound.
Although adults can develop T1D, and men are more at risk than women, it’s most prevalent among children, and it typically sets in at puberty. The rate of increase globally is at three percent annually among children.

Risk Factors
The risk factors are highly debatable in T1D, but it comes down to a few potential culprits.
- Genetics play a role if a child has beta-cell autoantibodies. This affects the way their bodies process glucose because the antibodies automatically destroy insulin or beta cells.
- According to Stanford Children’s Health, being Caucasian increases your risk of developing T1D, which is the opposite of T2D.
- Having cystic fibrosis, which causes scarring on the pancreas that stops the organ from producing insulin, also puts you at higher risk.
- Hemochromatosis, which causes an overload of iron that can damage the beta-pancreatic cells, is also a risk factor.
- Viral childhood infections can also cause T1D, such as rubella, measles, and mumps.
- Many other autoimmune disorders in which the immune system attacks organs such as the pancreas can lead to T1D. Examples of these disorders include celiac disease and thyroid autoimmune disease.
- Stress can lead to autoimmune dysfunction and the subsequent development of T1D.

T1D is a challenging condition that affects young and older people, but with proper care, frequent monitoring, and simple lifestyle changes, you can lead a pleasant life with the condition.
Common Symptoms
The symptoms of T2D can manifest in various ways, including:
- Increased urination
- Dehydration and thirst
- Increased appetite
- Blurry vision
- Unexplained fatigue
- Numbness or tingling in the hands and feet
- Wounds that take longer to heal
- Unexpected weight loss
- Thrush
Hyperglycemia is defined as high blood glucose levels. Patients with hyperglycemia exhibit dry mouth, nausea, vomiting, a fruity smell on the breath, difficulty breathing, and coma. Untreated hyperglycemia can be life-threatening.
Hypoglycemia is a potentially life-threatening condition of having extremely low blood glucose levels. Symptoms include shakiness, a pale face, sweating, chills, anxiety, and a rapid heartbeat.
The symptoms of hypoglycemia and hyperglycemia occur more commonly in T1D than T2D, and they are more severe in T1D.
Other hypoglycemic symptoms include dizziness, lightheadedness, nausea, weakness, extreme fatigue, tingling, and severe headaches. If untreated, patients can develop seizures, loss of consciousness, or coma.
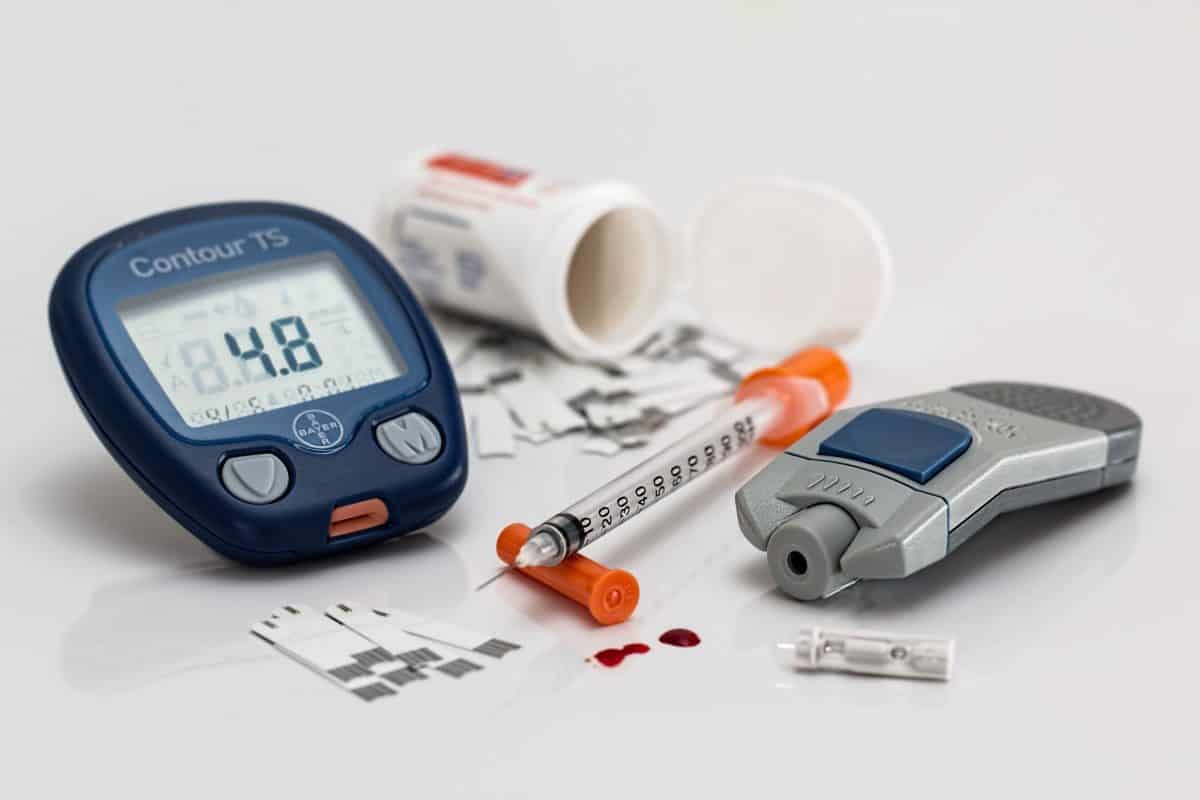
Can T2D Change Into T1D?
The simple answer is no. Even though the two main types of diabetes share similarities, they aren’t caused by the same factors.
Patients who suffer from an uncommon condition called latent autoimmune diabetes in adults (LADA) can be thought to have T2D when they actually have T1D.
LADA mimics T2D, but the fact that it is an autoimmune condition that prevents pancreatic cells from producing insulin makes it a T1D disorder. The LADA test establishes the diagnosis. So, to clarify again, T2D cannot become T1D.
Final Thoughts
Whichever type of diabetes you suffer from, you should adopt a healthier lifestyle to support treatment. Insulin-dependent individuals can’t simply throw out their injections. Instead, they should use lifestyle changes to improve their overall health while adequately treating their T1D.
T1D is undoubtedly stressful, but amazing advancements are being made that could change the way we treat it in the near future. Don’t give up hope, even if you have to rely on insulin.
References
https://www.cdc.gov/diabetes/basics/type2.html#:~:text=More%20than%2034%20million%20Americans,adults%20are%20also%20developing%20it
https://www.fda.gov/tobacco-products/health-information/cigarette-smoking-risk-factor-type-2-diabetes#:~:text=Smokers%20are%2030%20to%2040,type%202%20diabetes%20than%20nonsmokers.&text=Smoking%20can%20also%20make%20managing,to%20regulate%20blood%20sugar%20levels
https://portlandpress.com/biochemj/article-abstract/474/8/1321/49583/Vitamin-D-deficiency-and-diabetes?redirectedFrom=fulltext
https://www.stanfordchildrens.org/en/topic/default?id=type-1-diabetes-in-children-90-P01977
https://diabetes.diabetesjournals.org/content/54/suppl_2/S68


