Sleep. It’s embraced as a core pillar of health, equal to exercise, good nutrition, and regular check-ups with your doctor.
Table of contents
- Initial Visit
- Sleep Study Process
- HST Process
- Waiting for Results
- Obstructive Sleep Apnea Treatment
- What’s Sleep Apnea, and What’s Obstructive Sleep Apnea?
- Why Is Obstructive Sleep Apnea a Health Problem?
- How Does Medicare Cover My CPAP?
- What CPAP Devices will Medicare Cover?
- Will Medicare Cover CPAP Replacement Parts?
- Damaged or Lost CPAPs
- Why Pay for Sleep Studies and CPAPs?
- Is a CPAP Machine the only way to treat Sleep Apnea?
- Does Medicare Cover Other Sleep Disorders?
- How Do Medicare Advantage and Medigap Factor into this?
- Conclusion
You try to sleep, and maybe you do so for 8 or more hours if you’re 60 or older. Despite that, maybe you wake up with a host of problems.
Do you have painful headaches in the morning or are excessively sleepy during the daytime? Maybe you’re in situations where being sleepy could be potentially fatal, such as when driving. Over the past years, you may have noticed memory loss, decreased sex drive, constant irritability, or a complete lack of focus. Your partner may complain of constant mood swings or tell you that you snore so loudly that it can be heard throughout the house.
If you’re displaying the above symptoms and have been for the past few months, you shouldn’t hesitate to see a doctor–it could be urgent. You may have a sleep disorder, and promptly treating it will improve your overall health. Fortunately, those on Medicare are eligible for sleep studies that can diagnose sleep disorders.
Sleep disorders are numerous and complicated and are more likely to affect older adults. Your Medicare deductibles, copay, and responsibilities are determined by diagnosis methods, sleep disorder, and recommended treatment. But before you can get to all that, you must complete the first step: the sleep study.
Initial Visit
You’ve set up an appointment with a doctor who accepts Medicare. After you explain your symptoms, that doctor will order a “sleep study.” Note that if the only symptom you can bring up is snoring, you may not be eligible for a Medicare-covered sleep study. Additionally, snoring should not be the only tell-tale sign of a sleep disorder. Snoring tends to be more apparent in men with sleep disorders, whereas mood swings are more likely to appear in women with sleep disorders. To be eligible, you should explain how you believe your snoring (and sleep quality) affects you, such as fatigue or forgetfulness.
A sleep study is an examination to be taken, as the name suggests, while you’re asleep. When you’re asleep, you aren’t aware of your breathing, movements, and other actions. Through a sleep study, you undergo an exam that enables a doctor to monitor your brain and body activity while asleep.
Generally, sleep exams and treatments are covered under Medicare Part B. Under Part B, Medicare will cover either (1) medically necessary or (2) preventative services. You must first meet your Part B deductible to be eligible for Part B services. In 2019, that monthly deductible is $185.
Upon meeting your deductible, Medicare will cover 80% of the costs associated with your sleep-related treatment; you (or your other insurance) are responsible for the other 20%.
Sleep Study Process
Medicare will cover these sleep studies: Type I, II, III, and IV.
- Type 1: An exam done at a physical location, typically a sleep lab, is called a polysomnogram (“PSG”). At the sleep lab, a sleep technician will hook up various devices to you designed to measure factors such as airflow, respiratory effort, and oxygen saturation. Factors like these are called “sleep parameters” or “channels.” You then stay there the night. It may be difficult to fall asleep in that environment, but the plus side is that the lab will have data to work with immediately.
- Type II: This sleep study is done through a Home Sleep Test (“HST”). It can be performed at home and requires no attendance. This HST device will monitor 7 channels.
- Type III: HST device that will monitor 4 channels.
- Type IV: HST device that will monitor 1-2 channels.
If you are ordered a sleep study designed only for “naps” (short daytime sleep), that will not be covered under Medicare.
HST Process
Typically, a doctor will notify a sleep lab that you require a sleep study, and it is at their discretion on which sleep study is appropriate. If it is an HST, the sleep lab will arrange for the HST to be shipped to you. You’ll receive instructions on how to use it and your responsibilities. By responsibilities, this means financial obligations. Specifically, you may be hit with fees for each day you fail to ship the HST back past your study period or if you lose/break the device. Daily fees for failure to deliver could go to $150 a day and even to $2,500 if you lose or break the device.
An HST can be hooked up to your chest and has tubing to be placed in your nostrils. You will be instructed to sleep with it for a minimum of hours, the most common being at least 4+ hours. The device will account for breaks when you wake up, use the bathroom, or get water. Typically, you will be asked to keep the device on for two to three nights. When doing the HST, you’ll fill out papers with questions like what time you went to bed, what time you woke up, and whether you drank alcohol that night,
You’ll attach your completed paperwork and send the HST back to the lab.
Waiting for Results
Once the sleep lab completes either the PSG or receives the HST, you will need to wait. Sleep studies can output several thousand pages of data, which will need to be evaluated by a sleep doctor. This means a doctor licensed or associated with the American Academy of Sleep Medicine; this could also mean a doctor whose primary occupation is working in a sleep lab.
Based on your results, that sleep doctor will diagnose you with a sleep disorder and recommend the appropriate treatment. Medicare currently covers those diagnosed with sleep apnea, and there are three types: obstructive sleep apnea (“OSA”), central sleep apnea, and complex sleep apnea syndrome.
Obstructive Sleep Apnea Treatment
If you’ve been diagnosed with OSA, you can be prescribed a Continuous Positive Air Way Pressure machine or “CPAP.” Medicare Part B will cover Durable Medical Equipment (“DME”), and CPAPs are listed as eligible DME. You can also inquire about your eligibility for a Bilevel Positive Airway Pressure device (“BiPAP”), an OSA treatment device for those unable to tolerate CPAPs. BiPAP is designed with an additional pressure setting, using both an inhale and exhale pressure when you breathe,
You may be initially for a three-month trial period for CPAP therapy. If you opt for a CPAP, you will speak with your doctor regarding your OSA diagnosis. Medicare will then work with a Medicare-approved medical supplies provider and arrange for you to receive a CPAP. If it’s determined that CPAP therapy is helping you, then your trial period can be extended. Currently, Medicare will pay the medical supplier for CPAP rental for 13 months, and then the CPAP machine will be considered yours–you no longer pay fees to the supplier.
As previously stated, if you’ve met your Part B deductible, Medicare will cover 80% of the associated costs, and you’ll be responsible for the other 20%.
What’s Sleep Apnea, and What’s Obstructive Sleep Apnea?
Sleep apnea is a severe sleeping disorder and is likely to affect older Americans.
Apnea is the cessation of breathing. For those with OSA, your throat can be closed off during sleep. Hence the term sleeps apnea. To be diagnosed with sleep apnea, the sleep doctor will measure your sleep study results using an Apnea-Hypopnea Index (“AHI”). The AHI is the sum of the number of apneas (breathing pauses) and hypopneas (shallow breathing) that, on average, happen in one hour: these are called “events.” To be measured as AHI, either of these events must occur for at least 10 seconds. If you are under 5 AHI, you have no sleep apnea. If you are above 30, you have severe sleep apnea. With severe sleep apnea, the consequences can be devasting and should be brought up with your Medicare doctor.
Why Is Obstructive Sleep Apnea a Health Problem?
When you experience apnea, you begin to be starved of oxygen. Your brain will then wake you up to force you to breathe, interrupting your sleep. In OSA, those interruptions can cause many as 30 (or more) interruptions per sleep session. Additionally, constant apnea can result in the most common sign of OSA: loud snoring.
Uninterrupted sleep is essential to entering “deep sleep,” a stage of sleep necessary for the mind and body to recuperate and rebuild themselves each day. Without that, you can experience daytime fatigue, memory loss, poor emotional control, and an increased risk for heart disease. This is because the heart must exert more effort in getting oxygen to your brain. The earlier you can prevent this, the better it is for your heart health.
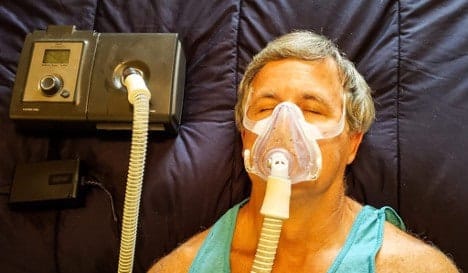
How Does Medicare Cover My CPAP?
With CPAP therapy, you will use your CPAP device each night, and it’s recommended you use it each time you sleep (even with naps). The CPAP places a certain amount of pressure on your airway via a mask. This pressure ensures your airways are open and you breathe properly while asleep. With a CPAP, you have a higher chance of entering deep sleep, and your health will begin to improve overall. You may notice that you have more energy, a better ability to focus at school or work, and a better capacity to handle your relationships.
What CPAP Devices will Medicare Cover?
Currently, there are no guidelines for the type of CPAP Medicare will cover. CPAPs are incredibly expensive and complicated DME. Modern CPAPs have minimal noise, along with many advanced features. These might include:
- An automatic feature that detects the degree of pressure needed to keep your AHI low (so you do not manually have to try figuring it out)
- Wireless functions or an SD card that keeps track of use, AHI, and amount of events per hour (data that can be used to show your doctor in case there are still problems)
- Automatic detection on how well your mask is sealed (when air escapes during use, this is called a “leak”) and whether CPAP parts need to be replaced
- A humidifier to prevent dry throat
- Automatic detection of when you’ve taken the mask off (so that it can automatically turn off
- Adjustable “ramp-up” times where the machine sets a default pressure, then increases it (as needed) once it detects you’re asleep; this is designed for comfort.
CPAPs can take some time to adjust to. After all, you are trying to sleep with a mask on your face. Remember to be patient and disciplined when starting CPAP therapy. Generally, CPAP users gain the most benefit when they can keep the CPAP on them for at least 4+ hours. If you can do that, your device may record that. If you wake up before 4 hours, you will need time to adjust to the CPAP and your preferred settings.
Will Medicare Cover CPAP Replacement Parts?
CPAP parts are disposable and will need to be replaced. One of these parts is the CPAP mask that comes with your machine. Depending on your specific needs, you will have either:
- a nasal pillow: a mask designed to go only into your nostrils
- a nasal mask: a mask designed to cover your nose
- a full-face mask: a mask designed to cover both your nose and your mouth
Always work with your medical supplier to ensure a properly sealed mask with 0 leaks. So long as you care for it and keep it washed, your mask will work for quite some time.
Medicare recommends that your mask be replaced every 3-6 months. Along with masks, your CPAP will come with “air filters,” which, as the name suggests, filter what you’re breathing in. This is especially important if you have a dusty home or pets that frequently shed. For filters, Medicare recommends a replacement every month. Medicare replacement schedules can be found on the CMS.gov website.
To schedule replacements, make sure that Medicare has a valid supply prescription on file. Afterward, you can try to make direct requests, but this would require you to keep track of Medicare’s replacement schedule. Alternatively, you can request regular mail deliveries, so you don’t have to worry about schedules. New CPAP models are released frequently, and Medicare recommends replacing your machine every five years.
As stated before, once you’ve met your Part B deductible, Medicare will cover 80% of the cost of your supplies, and you will be responsible for the other 20%.
Damaged or Lost CPAPs
If your CPAP is damaged, lost, or faulty, you must contact Medicare regarding eligibility and costs for replacements/repairs. Depending on the situation, Medicare will cover the cost to replace or repair your equipment and cover the cost of renting equipment while the originals are being repaired.
Why Pay for Sleep Studies and CPAPs?
For Americans on Medicare, the benefits of CPAP therapy often outweigh your deductible costs, plus a 20% copayment for sleep studies, CPAP equipment, and CPAP replacement parts. As you use your CPAP, you’ll have a wide range of long-term benefits such as:
- Reduced risk of heart problems like congestive heart failure and coronary artery disease
- Reduced risk of stroke
- Reduced risk for Type 2 Diabetes
- Reduced risk of causing motor vehicle accidents
You’re also likely to experience the following physical benefits:
- Increased daytime alertness
- Reduced or eliminated snoring
Additionally, untreated, severe sleep apnea can cause serious damage to brain tissue over time. Those undergoing CPAP therapy will begin to develop a more regular sleeping pattern and ensure that the amount they sleep is quality sleep (e.g., entering “deep sleep”), thereby repairing the damage done to their brain. It would help if you didn’t rule out being able to experience improvements to your well-being in these ways:
- Increased concentration
- Improved productivity
- Decreased chances of making mistakes at school or work
- Increased emotional stability
- Improved memory
- Better relationships with your partner through (1) improved mood, (2) reduction in irritability, (3) reduction in depressive symptoms, and (4) finally, letting your partner get quality sleep without being disturbed by snoring.
As you can see from the above, the costs of untreated sleep disorders will result in even more health problems. And more health problems lead to even more deductibles (because you may need to take on other plans) and even more copayments. Consider viewing the costs of your Medicare deductibles and copayments as a preventative measure against even further debilitating conditions. Your sleep troubles may not be fatal to you in the short term. Still, they can certainly become that way in the long term, either through chronic conditions, inability to work, or inability to have stable relationships.
If you’re an older American, age 60 or older, unsure if it’s worth the cost to undergo sleep studies, you will still highly benefit. Regardless of age, every Medicare patient benefits substantially from improved sleep and oxygen flow.
The process from a sleep study to diagnosis to receiving your DME can take months–and those are months you will still suffer from the damages of poor sleep. If you’re on Medicare, it’s highly advised to promptly seek out your primary care physician and request a sleep study.
Is a CPAP Machine the only way to treat Sleep Apnea?
Though CPAPs are the standard for sleep apnea treatment, alternative treatments are available. If your doctor determines that you cannot tolerate a CPAP, that doctor can prescribe you a specially-made oral mouthpiece. As with the CPAP, Medicare requires you to meet the same criteria of meeting with a Medicare-approved doctor and undergoing a sleep study. If you are approved for an oral device, you will need to receive it from a dentist who is a licensed Medicare DME supplier.
Does Medicare Cover Other Sleep Disorders?
Currently, Medicare covers sleep studies if you exhibit symptoms of OSA, but those can also overlap with symptoms of other sleep disorders. Your doctor can prescribe medication if you’re diagnosed with narcolepsy or insomnia. For medication, you will need to be enrolled in a Medicare Part D Drug Plan, which you can be enrolled in on its own, or as an additional Plan with your other Medicare Coverage (e.g., Part A or Part B). Under Part D, you’ll need to meet the current monthly deductible of $415.
Your copay will depend on the drug you’re being prescribed. Prescription drugs as listed in a “drug formulary,” categorizing drugs into different tiers. Drugs in Tier 1 are for generics and have lower copayments. Tiers 2 to 5 are brand-name and specialty drugs requiring higher out-of-pocket payments.
How Do Medicare Advantage and Medigap Factor into this?
The article uses ” Medicare ” to refer to “Original Medicare.” If you have a Medicare Advantage Plan, your sleep studies and requisite treatments are covered since Medicare Advantage Plans (also known as Medicare Plan Part C) must have Original Medicare’s Part A and Part B coverage. The benefit of this is that your plan may even include prescription drug coverage if you require drugs to treat your sleep disorder. If you have Medigap, you can use it as a source for you to cover the other 20% of your Part B copayments.
Conclusion
To wrap this up, If lack of energy, emotional instability, or decreased cognitive performance interfere with your life–don’t wait. “Doing Nothing” is the worst option for your sleep, and if you’re on Medicare and capable of meeting your monthly deductibles, then there’s no reason to delay. Schedule an appointment with your Medicare-approved doctor today and ask for a sleep study: it could save your life.
If you qualify for Medicare but don't know where to start, we have licensed insurance agents ready to answer your questions and help you enroll in Medicare Advantage, Medicare Supplement Insurance, and Prescription Part D plans.