Hormone replacement therapy (HRT) has helped millions of women navigate the challenges of menopause and hormonal changes. If you’re experiencing hot flashes, night sweats, mood changes, or other symptoms of hormone decline, understanding your treatment options is the first step toward feeling like yourself again.
This comprehensive guide covers everything you need to know about HRT, from how it works to potential benefits and risks, helping you make an informed decision about whether it’s right for you.
Article Contents
What is Hormone Replacement Therapy?
Hormone replacement therapy is a medical treatment that supplements or replaces hormones your body no longer produces in adequate amounts. As women approach menopause, typically in their late 40s or early 50s, the ovaries gradually produce less estrogen and progesterone. This natural decline triggers a cascade of symptoms that can significantly impact quality of life.
HRT works by reintroducing these hormones into your system, either through estrogen alone (for women who’ve had a hysterectomy) or a combination of estrogen and progesterone (for women with an intact uterus). The treatment can alleviate many menopause symptoms while also providing protective benefits for bone health and cardiovascular function when started at the appropriate time.
The decision to start HRT is highly personal and should be made in consultation with a healthcare provider who understands your medical history, risk factors, and treatment goals. Getting started with HRT is now easier than ever with telemedicine platforms like DirectCare.ai, which connects you with experienced providers who can evaluate your symptoms and create a personalized treatment plan from the comfort of your home.
Types of Hormone Replacement Therapy
Understanding the different types of HRT helps you have more productive conversations with your healthcare provider about which option might work best for your situation.
Estrogen-Only HRT
This type of HRT is typically prescribed for women who have had a hysterectomy (surgical removal of the uterus). Since there’s no risk of uterine cancer without a uterus, these women can safely take estrogen alone, which is the most effective treatment for menopause symptoms.
Estrogen-only therapy comes in several forms including pills, patches, gels, creams, and vaginal preparations. The delivery method affects how the hormone is absorbed and metabolized, which can influence both effectiveness and side effect profiles.
Combined HRT (Estrogen + Progesterone)
Women who still have their uterus need progesterone along with estrogen. This combination is crucial because estrogen alone can cause the uterine lining to thicken excessively, increasing the risk of endometrial cancer. Progesterone protects the uterus by preventing this overgrowth.
Combined HRT can be taken in several ways: – Continuous combined: Taking both hormones daily with no breaks – Sequential combined: Taking estrogen daily with progesterone added for part of each month – Continuous long-cycle: Taking estrogen daily with progesterone every three months
Bioidentical vs. Synthetic HRT
Bioidentical hormones are chemically identical to the hormones your body produces naturally, while synthetic hormones have a slightly different molecular structure. Both types are created in laboratories—“bioidentical” doesn’t mean natural or plant-derived, though some are sourced from plant compounds.
The debate over bioidentical versus synthetic HRT continues, with advocates on both sides. What matters most is finding a formulation that effectively manages your symptoms with minimal side effects, which is where personalized medical guidance becomes essential.
The Benefits of HRT
HRT offers numerous benefits beyond symptom relief. Understanding these advantages helps you weigh the potential value against any risks.
Immediate Symptom Relief
The most noticeable benefits appear within weeks to months of starting treatment:
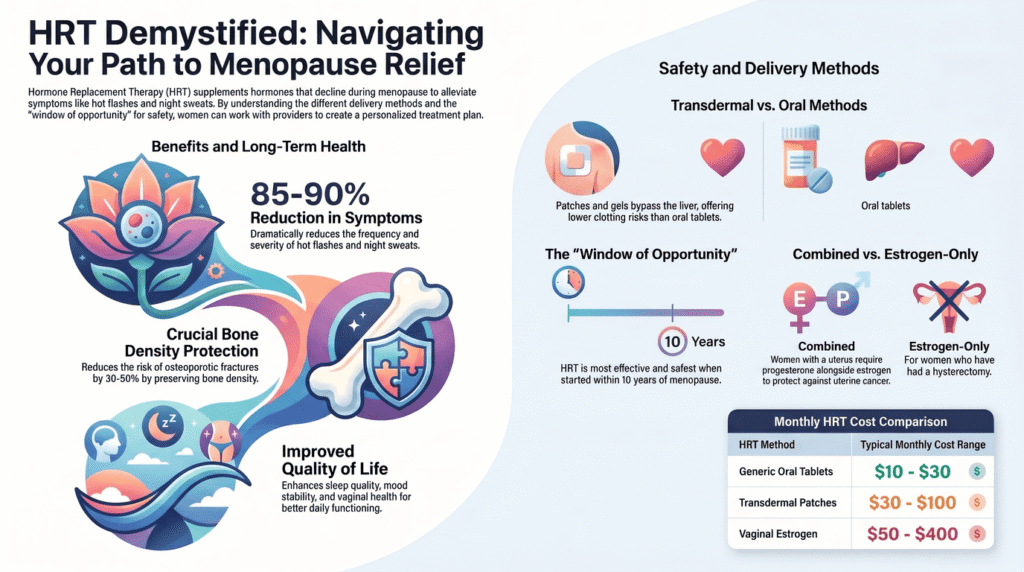
Hot Flashes and Night Sweats: HRT reduces the frequency and severity of vasomotor symptoms by up to 85-90%. Many women report dramatic improvements in sleep quality once night sweats subside, which positively affects energy, mood, and cognitive function.
Sleep Disturbances: Better sleep is one of the most life-changing benefits women report. When you’re not waking up drenched in sweat multiple times per night, your body can complete proper sleep cycles, leading to better mental clarity and emotional stability.
Vaginal and Urinary Symptoms: Estrogen prevents vaginal atrophy (thinning and drying of vaginal tissues), reducing discomfort during intercourse, urinary urgency, and recurrent infections. This aspect of HRT can significantly improve intimate relationships and overall comfort.
Mood Changes: While HRT isn’t a treatment for clinical depression, many women notice improved mood stability, less irritability, and reduced anxiety when hormone levels stabilize. The improvement in sleep quality also contributes to better emotional regulation.
Long-Term Health Protection
Beyond symptom management, HRT provides important protective benefits when started during the “window of opportunity” (typically within 10 years of menopause onset or before age 60):
Bone Health: Estrogen plays a crucial role in maintaining bone density. Women can lose up to 20% of bone density in the first five years after menopause, significantly increasing fracture risk. HRT effectively preserves bone density and reduces the risk of osteoporotic fractures by 30-50%.
Cardiovascular Benefits: When started early in menopause, HRT may offer cardiovascular protection, though this benefit is timing-dependent. Recent research suggests that women who start HRT within 10 years of menopause may have reduced risk of heart disease compared to those who don’t use HRT.
Cognitive Function: Some studies suggest HRT may support cognitive function and potentially reduce dementia risk when started during the menopausal transition, though research is ongoing in this area.
If you’re experiencing menopause symptoms and wondering whether HRT could help, DirectCare.ai offers convenient virtual consultations with providers who specialize in women’s hormone health. Their telehealth platform makes it easy to discuss your symptoms, get lab work ordered if needed, and receive a personalized treatment recommendation.
How to Get Started with HRT
Beginning HRT involves several steps to ensure the treatment is safe and appropriate for your specific situation.
Initial Consultation
Your journey starts with a comprehensive medical evaluation. Your healthcare provider will review:
- Your complete medical history, including any history of blood clots, heart disease, stroke, or hormone-sensitive cancers
- Current medications and supplements
- Family history of breast cancer, ovarian cancer, or cardiovascular disease
- Severity and impact of your menopause symptoms
- Your treatment goals and concerns
This conversation helps your provider assess whether HRT is appropriate and which type might work best for you.
Lab Testing and Assessments
While menopause is often diagnosed based on symptoms and age, some situations warrant hormone level testing:
- Women experiencing premature menopause (before age 40)
- Unclear diagnosis or atypical symptoms
- Specific medical conditions requiring baseline measurements
Additional tests might include mammography, lipid panels, blood pressure checks, and bone density screening, depending on your age and risk factors.
Choosing Your HRT Regimen
Your provider will recommend a specific hormone type, dose, and delivery method based on:
- Whether you have a uterus (determining estrogen-only vs. combined therapy)
- Your symptom severity
- Personal preferences regarding administration method
- Medical conditions that might favor one delivery method over another
- Cost and insurance coverage considerations
Most providers follow the principle of using the lowest effective dose for the shortest necessary duration, though many women safely use HRT for many years.
Monitoring and Adjustments
HRT isn’t a “set it and forget it” treatment. Expect follow-up appointments at:
- 3 months: Assess initial response, side effects, and need for dose adjustments
- 6-12 months: Evaluate ongoing effectiveness and any concerns
- Annually: Comprehensive review including mammogram reminders and health screenings
Finding the right HRT regimen sometimes requires patience and adjustments. With DirectCare.ai, follow-up consultations are straightforward and convenient, allowing you to discuss how you’re responding to treatment without the hassle of scheduling in-person appointments weeks in advance.
HRT Delivery Methods
The way you take HRT significantly affects how your body processes the hormones, which can influence both effectiveness and side effects.
Oral Tablets
Pills are the most common form of HRT. You take them daily, typically at the same time each day for consistency.
Advantages: – Convenient and familiar – Well-studied with decades of data – Often covered by insurance
Considerations: – Pass through the liver (first-pass metabolism), which affects clotting factors – May not be ideal for women with certain liver conditions or increased clotting risk – Can affect cholesterol levels (sometimes beneficially)
Transdermal Patches
Patches deliver hormones through your skin directly into the bloodstream, bypassing the liver.
Advantages: – Avoid first-pass liver metabolism – Steady hormone levels with fewer peaks and valleys – Lower risk of blood clots compared to oral HRT – Only need changing once or twice weekly
Considerations: – Can cause skin irritation at application site – Visible on skin (though newer patches are quite discreet) – May not stick well if you exercise heavily or live in humid climates
Topical Gels and Creams
These are applied daily to the skin, usually on the arms, shoulders, or thighs.
Advantages: – Flexible dosing adjustments – Avoid liver metabolism like patches – No visible patch
Considerations: – Must be applied daily – Need to let dry before dressing or contact with others – Potential for transfer to partners or children through skin contact
Vaginal Preparations
Low-dose estrogen creams, tablets, or rings inserted into the vagina treat local symptoms effectively.
Advantages: – Highly effective for vaginal and urinary symptoms – Minimal systemic absorption with low-dose preparations – Can be used alone or combined with systemic HRT
Considerations: – Doesn’t address hot flashes or other systemic symptoms – Requires vaginal application (though rings stay in place for months)
Other Methods
Additional options include vaginal rings (systemic), skin sprays, and subcutaneous pellets, though these are less commonly used.
Understanding the Risks of HRT
No medical treatment is without risks, and HRT has received considerable attention regarding potential health concerns. Understanding these risks in context helps you make informed decisions.
Breast Cancer Risk
The relationship between HRT and breast cancer is complex and depends on multiple factors:
- Type of HRT: Estrogen-only therapy shows little to no increased breast cancer risk and may even reduce it slightly. Combined HRT (estrogen plus progesterone) shows a small increased risk that becomes detectable after about 5 years of use.
- Duration: Risk increases with longer duration of use, particularly beyond 5-10 years.
- Baseline risk: Your personal breast cancer risk before starting HRT matters significantly. Women with family history or other risk factors need more careful consideration.
The absolute risk increase is small—roughly an additional 1-2 breast cancer cases per 1,000 women using combined HRT per year. For context, obesity, excessive alcohol use, and lack of exercise each carry similar or greater breast cancer risks.
Cardiovascular Risks
HRT’s effect on heart health is highly timing-dependent:
- Early initiation: Starting HRT within 10 years of menopause (or before age 60) appears neutral or potentially protective for heart health.
- Late initiation: Starting HRT more than 10 years after menopause increases cardiovascular risk and is generally not recommended.
- Delivery method: Transdermal HRT (patches, gels) carries lower clotting and stroke risk than oral HRT.
Women with existing cardiovascular disease, history of blood clots, or multiple risk factors require careful evaluation before starting HRT.
Blood Clot Risk
Oral estrogen increases the risk of venous thromboembolism (blood clots in legs or lungs), particularly in the first year of use. This risk is higher for women who:
- Are overweight or obese
- Smoke
- Have a personal or family history of blood clots
- Have clotting disorders
- Are immobile for long periods
Transdermal HRT (patches and gels) doesn’t increase clotting risk and is the preferred choice for women with elevated risk factors.
Stroke Risk
The stroke risk associated with HRT is small but increases with age and in women with cardiovascular risk factors. Again, transdermal preparations carry lower risk than oral forms.
Putting Risks in Perspective
For healthy women starting HRT during the appropriate window (within 10 years of menopause or before age 60), the absolute risks are quite small, especially when weighed against the quality-of-life benefits and bone protection HRT provides.
Your personal risk profile determines whether HRT is appropriate for you. DirectCare.ai providers conduct thorough risk assessments during consultations to ensure HRT is safe for your individual situation, taking into account your complete medical history and risk factors.
Who Shouldn’t Take HRT?
While HRT is safe for many women, certain conditions make it inappropriate or require extreme caution:
Absolute contraindications: – Known or suspected breast cancer – Other hormone-sensitive cancers – Undiagnosed vaginal bleeding – Current or history of blood clots – Active liver disease – History of heart attack or stroke – Known pregnancy
Relative contraindications (requiring careful evaluation): – Endometriosis – Uterine fibroids – Gallbladder disease – Migraine with aura – Strong family history of breast cancer – Elevated cardiovascular risk
If you have any of these conditions, discuss alternatives with your healthcare provider. Low-dose vaginal estrogen, non-hormonal medications, or lifestyle modifications might be appropriate alternatives.
Alternatives to HRT
If HRT isn’t suitable for you, or you prefer to try other approaches first, several alternatives exist:
Non-Hormonal Medications
- SSRIs/SNRIs: Low-dose antidepressants can reduce hot flashes by 40-60%
- Gabapentin: An anti-seizure medication effective for hot flashes
- Fezolinetant (Veozah): A newer non-hormonal medication specifically for hot flashes
- Vaginal moisturizers: Over-the-counter products for vaginal dryness
Lifestyle Modifications
- Layered clothing and breathable fabrics
- Maintaining healthy weight
- Regular exercise
- Stress reduction techniques
- Avoiding triggers (spicy food, alcohol, caffeine)
- Maintaining cool bedroom temperature
Complementary Approaches
- Cognitive behavioral therapy for managing symptoms
- Clinical hypnotherapy
- Acupuncture (some evidence for hot flash reduction)
Supplements
While popular, most supplements lack strong evidence for menopause symptoms. Some women report benefits from: – Black cohosh – Soy isoflavones – Red clover
Always discuss supplements with your provider as they can interact with medications.
Cost of HRT
HRT costs vary significantly based on type, dosage, and whether you have insurance coverage.
Typical monthly costs: – Generic estrogen pills: $10-30 – Brand-name estrogen pills: $50-200 – Patches: $30-100 – Gels: $50-200 – Vaginal estrogen: $50-400 – Compounded bioidentical hormones: $100-500+
Additional costs: – Initial consultation: $100-300 (or insurance copay) – Follow-up visits: $50-150 each – Lab tests: $50-300 depending on what’s tested – Annual monitoring and screenings
Most insurance plans cover FDA-approved HRT formulations, though you may pay less with generic versions. Compounded bioidentical hormones are typically not covered by insurance and cost significantly more.
Prescription discount programs like GoodRx can reduce costs substantially if you’re paying out of pocket or if the discount price is lower than your insurance copay.
How Long Should You Take HRT?
The duration of HRT use is highly individual and depends on your goals, response to treatment, and personal risk factors.
Current guidelines suggest: – No arbitrary time limits for women who benefit from HRT – Regular reassessment (at least annually) of continuing need – Lowest effective dose – Discontinuation if risk factors change significantly
Many women use HRT for 5-10 years or longer. Some stop once symptoms resolve, while others continue long-term for quality of life and bone protection. Women who stop HRT may experience symptom recurrence, though symptoms are often less severe than originally.
The decision about duration should be made collaboratively with your healthcare provider based on your ongoing symptom management needs and health status.
Making Your Decision
Deciding whether to start HRT requires weighing multiple factors:
Consider HRT if you: – Have moderate to severe menopause symptoms affecting quality of life – Are within 10 years of menopause or under age 60 – Don’t have contraindications – Are at increased risk for osteoporosis – Have tried lifestyle modifications without sufficient relief
Take more time to decide if: – Your symptoms are mild and manageable – You’re more than 10 years past menopause – You have significant risk factors for breast cancer or cardiovascular disease – You haven’t tried lifestyle modifications or non-hormonal options
Remember, starting HRT doesn’t lock you in permanently. You can try it and stop if it doesn’t work for you or causes unacceptable side effects. Most women who try HRT find significant relief and improved quality of life.
Conclusion
Hormone replacement therapy remains one of the most effective treatments for menopause symptoms, offering rapid relief from hot flashes, night sweats, and other changes that can significantly impact daily life. When started at the appropriate time and used with careful medical supervision, HRT also provides important protective benefits for bone health.
The key is finding a healthcare provider who takes time to understand your individual situation, discusses both benefits and risks thoroughly, and creates a personalized treatment plan that aligns with your health goals and concerns.
Modern telemedicine has made accessing knowledgeable HRT providers easier than ever. DirectCare.ai specializes in women’s hormone health and offers comprehensive virtual consultations, making it simple to get expert guidance on whether HRT is right for you—no matter where you live.
Your menopause journey doesn’t have to mean suffering through symptoms or accepting a diminished quality of life. With the right information and medical support, you can make confident decisions about managing this transition and maintaining your health and vitality for years to come.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider before starting, stopping, or changing any medication or treatment. Individual results may vary.
Affiliate Disclosure: This article contains affiliate links. We may earn a commission if you click through and make a purchase, at no additional cost to you.




