The elderly population is already at greater risk for several health conditions, diseases, and disorders, with many of them causing specific consequences related to skin health and integrity.
Due to consequences secondary to vascular disease and diabetes and nursing home complications, wounds and the need for wound care are becoming more common in the geriatric population.
Although the exact prevalence is difficult to measure because of inaccurate reporting and elderly individuals avoiding medical attention, it’s evident that the rates of wound development in the elderly are increasing.
In what follows, we’ll discuss several types of old wounds, some of which are more common than others. Further, we’ll outline some effective treatment options for such conditions. Finally, we’ll define wound care centers’ role while providing a general long-term outlook for recovery.
Common Types of Elderly Wounds
The prevalence of old wounds varies on the age of the individuals and whether or not they reside in a nursing home. However, wounds, such as ulcers, are more common in those older than 65 and tend to be more complicated in individuals living in nursing homes.
A study from a 2007 European survey suggested that the prevalence of pressure ulcers is about 18% among the older population.
The following are some of the common types of wounds in the elderly:
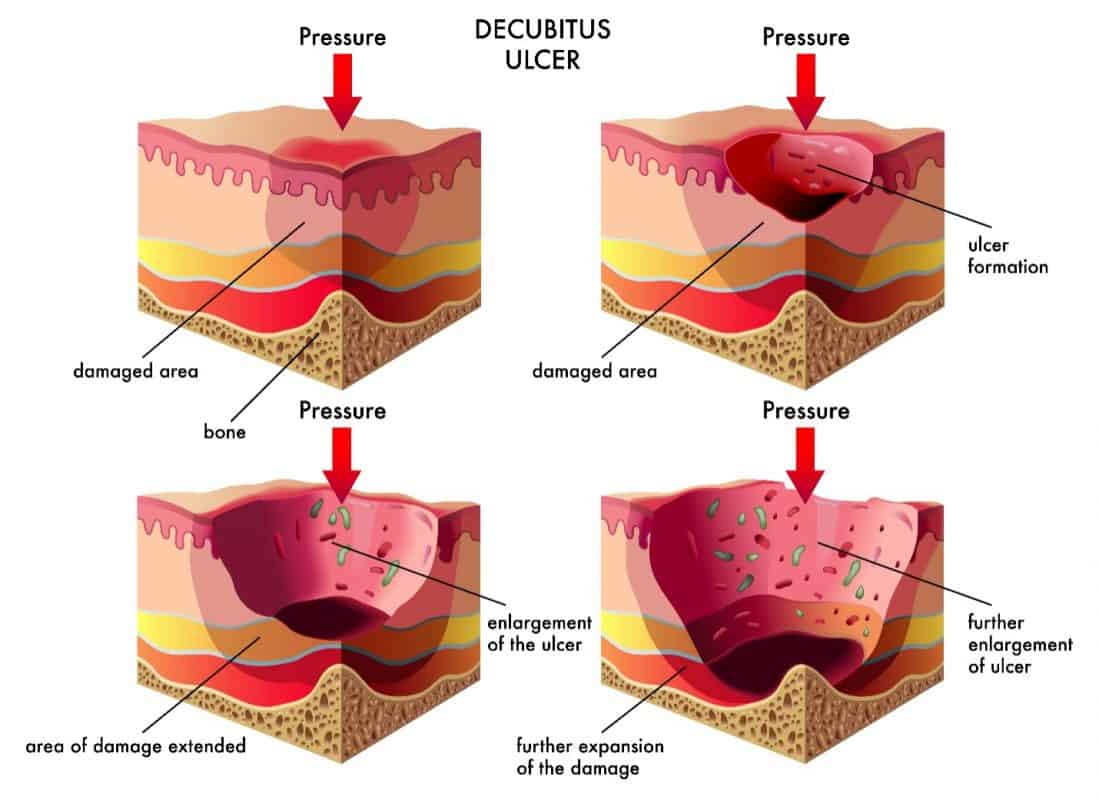
• Decubitus Ulcers of the Buttocks
• Diabetic Foot Ulcers
• Venous Stasis Ulcers
• Neuropathic Ulcers
• Arterial Insufficiency Ulcers

Many elderly wounds are caused by an imbalance in pressure points on the body, mainly when sleeping or sitting. The most common areas of the body affected are the tailbone, buttocks, legs, and back of the shoulder blades. In addition, issues with pressure points leading to ulcers can be secondary to decreased sensation, such as in neuropathic ulcers and chronic pressure on a specific area due to a lack of mobility of an individual.
Some of the most common risk factors for wounds, particularly pressure wounds, include malnutrition, dehydration, diabetes, infection, incontinence, and environmental contributions such as moisture buildup and friction.
While prevention can be difficult, especially in geriatrics, optimizing living environments, mainly sleeping settings, reduces the risk of discomfort, friction, and infection.
Though some types of geriatric wounds can recover, many have difficulty healing, and the individual may live with the damage chronically. For example, pressure ulcers, diabetic ulcers, ischemic ulcers, and venous ulcers are all examples of difficult-to-heal wounds.
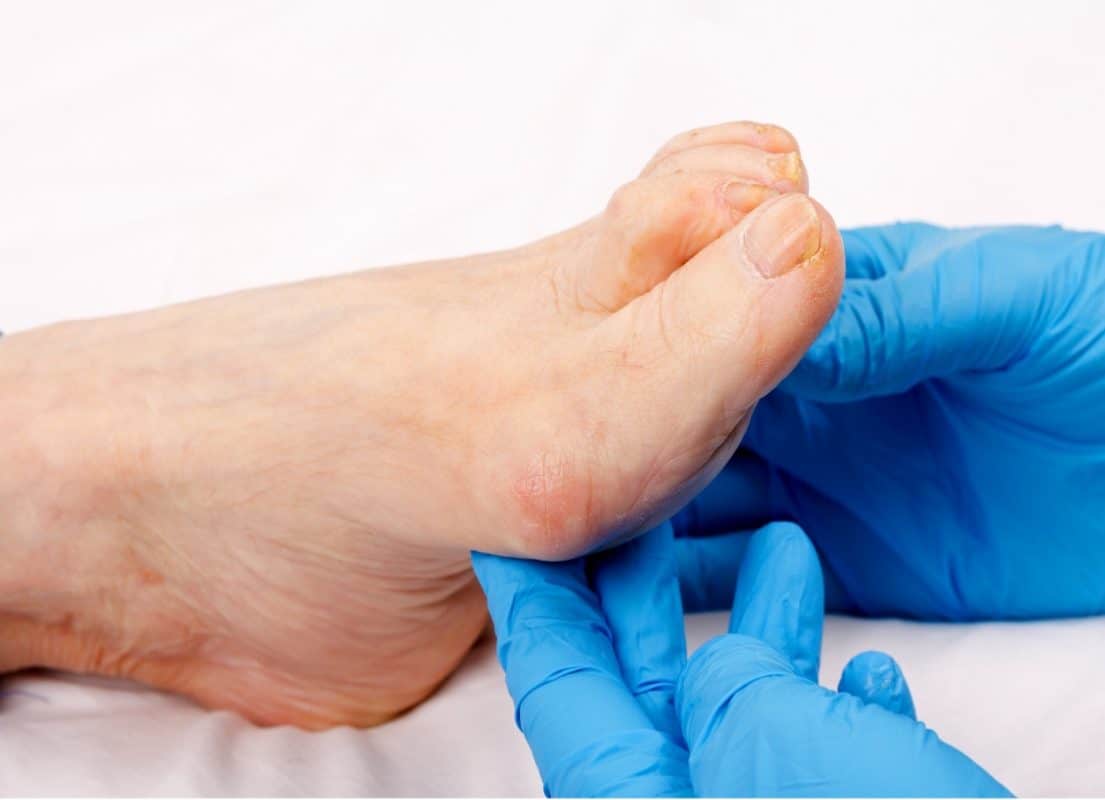
Wound Treatment and Management Protocols in The Elderly
Treating the several types of ulcer-derived wounds as discussed above requires a staging process that identifies the depth of the injury and the amount of healing that has occurred.
Depending on the stage of a particular wound, treatment may involve a variety of protocols, including topical ointments, systemic agents, wound coverage using various dressings, and surgical flaps to cover the area. Often this type of flap surgery is performed by a plastic surgeon, and the surgical technique can be pretty complex. For example, a wound that is quite large and is not amenable to simple closure or skin grafting may be an appropriate wound to consider a surgical flap to achieve wound coverage and closure.
Another example is the treatment of venous stasis ulcers by an Unna boot, a compression dressing containing zinc that helps protect and promote healing of the underlying venous ulcer. It would be best if you changed this dressing every few days.
Whether you visit your primary care physician, emergency, or a wound care center, their primary role is to evaluate the wound, identify its specific stage, and develop a treatment plan that is most suitable for the individual.
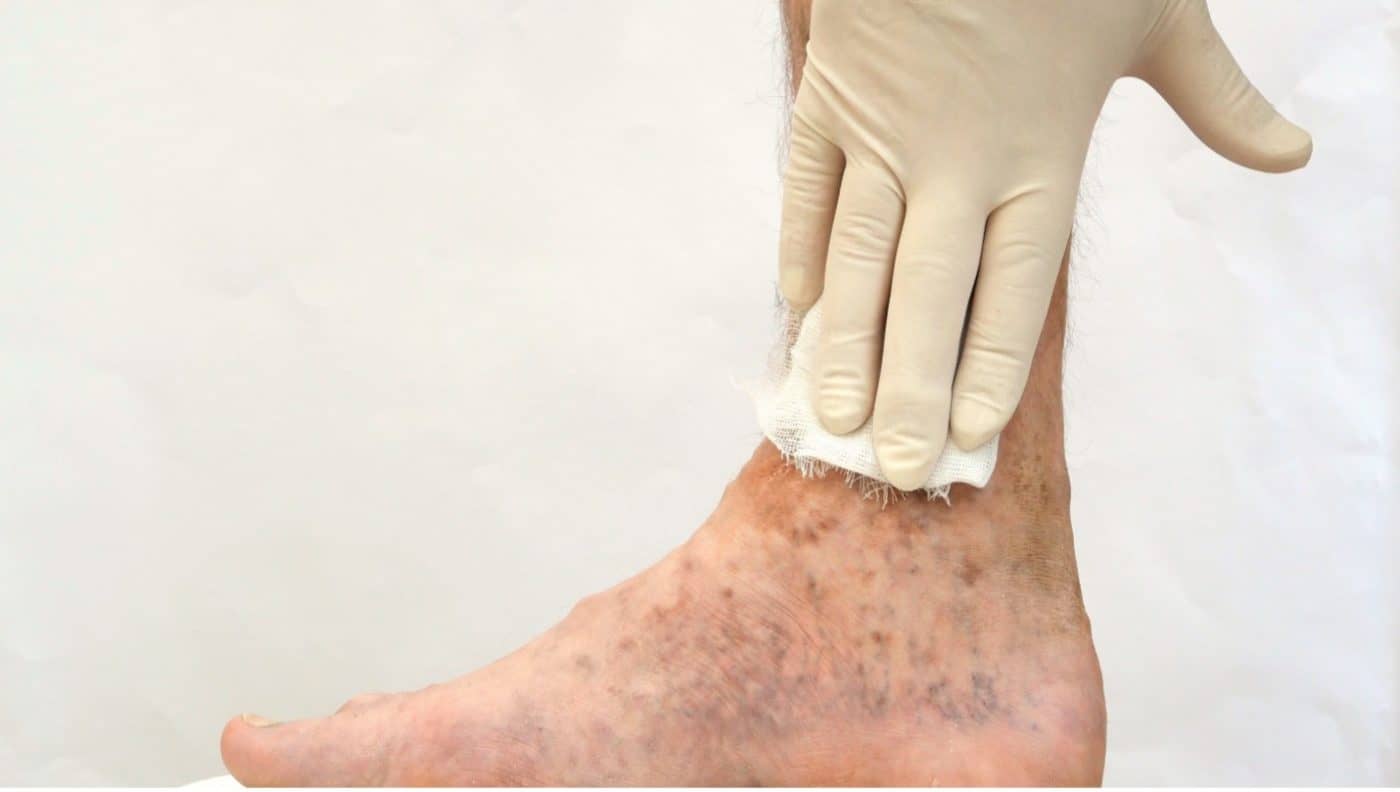
Other treatment considerations for treating different types of wounds include:
- Negative pressure wound therapy.
- Hyperbaric oxygen therapy.
- Electrical stimulation.
- Ultrasounds.
- Lifestyle interventions such as nutritional improvements to a patient’s diet.
Again, because many geriatric wounds are chronic, the approach to treatment and management is comprehensive and multidisciplinary, requiring efforts and expertise from physicians, physical therapists, occupational therapists, dieticians and nutritionists, nursing staff, social workers, surgeons, and even dermatologists.
The emergence of wound care centers has been highly beneficial for individuals with all types of wounds, and they have become trendy due to the focus on the best possible treatment for injuries.

Conclusion
The prevalence of chronic wounds is increasing in the elderly population and significantly impacts their quality of life. In addition, the older population is often more susceptible to injuries that have slower healing times and require prolonged treatment.
If treated promptly and effectively, the long-term outlook of geriatric wounds is optimistic. Although it may impede the patient’s quality of life in the short term, excellent wound care can result in the complete healing of wounds, which is the ultimate desired outcome.